Our webinar about Bladder Problems at Menopause featured WellFemme’s Dr Kelly Teagle and pelvic floor physiotherapist Marita O’Shea.
The following is a summary of the relevant information, as well as a list of excellent resources for further reading about particular bladder problems.
How Common Are Bladder Problems At Menopause?
VERY common! Australian statistical data from the Continence Foundation notes that:
- Urinary incontinence affects up to 13% of Australian men and up to 37% of women.
- 50% of women aged 45-59 had some degree of urinary incontinence over a 3-month period.
- 70% of people with urinary leakage do not seek advice or treatment.
[The following few sections are excerpts from Jean Hailes’ excellent “Bladder Incontinence” resource]
What is normal bladder function?
According to the Continence Foundation of Australia, a normal bladder:
- Empties 4-8 times each day (every 3-4 hours)
- Can hold up to 400-600ml of urine (the sensation of needing to empty occurs at 200-300ml)
- May wake you when it is full, but gives you enough time to find a toilet, and
- Does not leak urine.
Bladder incontinence – types and symptoms
| Types of incontinence | Signs and symptoms |
| Urge incontinence (urinary) | Bladder muscle contracts with little warning; you may feel:
|
| Stress incontinence (urinary) | Urine leaks when you exert yourself, such as when you sneeze, cough, laugh or jump, due to mobility in the bladder neck because of a weak pelvic floor. |
| Mixed incontinence | You experience both urge and stress symptoms. |
| Overflow incontinence | Occurs when the bladder fails to empty properly, becomes over-full and then tends to leak – it may be caused by poor contraction in the bladder muscle or by certain neurological or medical conditions, such as diabetes. |
Causes of incontinence
The pelvic floor muscles – the ‘sling’ of muscles that supports the bladder, bowel and uterus – can stretch and weaken, leading to continence issues. 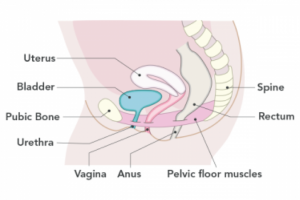 The following may also contribute to incontinence:
The following may also contribute to incontinence:
- pregnancy and childbirth
- being overweight
- chronic constipation that causes you to strain
- chronic coughing
- chronic back pain
- frequent lifting of heavy objects, including children and weights at the gym
- reduction in the hormone oestrogen after menopause
- some medications
- diabetes
- pelvic or abdominal surgery
- caffeinated drinks.
What Is An “Overactive Bladder”?
One of the most common bladder problems at menopause is Overactive bladder (OAB): urinary urgency, usually accompanied by frequency and nocturia, with or without incontinence. With OAB you will suddenly have the urge to rush to the toilet with little or no warning, and you may experience a small or large amount of leakage if the urge isn’t controlled. The urge is often in response to “trigger” situations, like putting the key into the front door when you arrive home, or fiddling with the buttons to get your pants down.
How Do Hormonal Changes Affect The Bladder?
Before menopause, a steady supply of estrogen helps preserve the strength and flexibility of your supportive pelvic and bladder tissues. During perimenopause and menopause, your estrogen levels drop dramatically. This can cause your tissues to weaken. Low estrogen levels may also contribute to a weakening in muscular pressure around your urethra. Changes in hormone levels may also increase the risk of urinary tract infections (UTIs) during perimenopause and menopause. UTIs may have similar symptoms as OAB.
What Type Of Bladder Issue Do I Have?
In order to work out what type of bladder problem you have your doctor will ask a lot of questions about how, when and how much you urinate or leak. They will need to know about your other medical issues and medications. They may also check for UTI’s and ask you to complete a bladder diary; this is a record of how much you drink and urinate, and when. Your doctor may examine you, or recommend that you be assessed by a continence/ pelvic floor physiotherapist (like Marita). The examination usually involves a bimanual examination, where the health worker inserts their gloved fingers into your vagina to assess the strength and state of your pelvic floor. You may also be referred for a urodynamic study; a specialist doctor used a tiny tube (catheter) inserted into your urethra to fill the bladder, and then test the pressure and holding capacity of your bladder.
How Are Bladder Problems Around Menopause Treated?
FIRST LINE:
- Fluid restriction
- Quit smoking
- Avoid irritants in diet
- Weight reduction
- Regulating bowel function
- Behavioural treatments
- Bladder training
Check out our webinar video above for Marita’s tips on behavioural management, bladder training and more! MEDICAL TREATMENTS FOR OAB:
- Bladder relaxants eg. Oxybutynin (eg. Ditropan), solifenacin (eg. VESIcare), tolterodine. Mirabegron (Betmiga), some antidepressants.
- Common side effects: constipation, dry mouth
- Estrogen- transvaginal (and/ or systemic)
- Botox injections
- Sacral nerve stimulation
- Bladder augmentation cystoplasty (surgery to enlarge bladder)
REFERENCES:
Australasian Menopause Society:
https://www.menopause.org.au/hp/studies-published/610-oestrogens-and-overactive-bladder
https://www.menopause.org.au/health-info/fact-sheets/urinary-incontinence-in-women
The Royal Australian College of GP’s:
https://www.racgp.org.au/afp/2012/november/overactive-bladder-syndrome/
Continence Health Australia:
https://www.continence.org.au/ https://www.continence.org.au/about-continence/continence-health/bladder
Jean Hailes information about bladder incontinence:
https://www.jeanhailes.org.au/health-a-z/bladder-bowel/bladder-incontinence
Healthline:
https://www.healthline.com/health/menopause/overactive-bladder-menopause
A DIY Bladder Diary:
https://www.continence.org.au/resource/bladder-diary-instructions _______________________________________________________________________________________________________________________________________________
What is WellFemme About?
If you can’t find the professional help you need for your peri/menopausal symptoms then book a telehealth consultation with an expert WellFemme menopause doctor.
WellFemme is Australia’s first dedicated Telehealth menopause clinic, servicing locations nationwide including: Melbourne, Sydney, Adelaide, Darwin, Perth, Hobart, Brisbane, Dubbo, Bendigo, Broken Hill, Broome, Alice Springs, Launceston, Cairns, Mildura, Lightning Ridge, Kalgoorlie, Albany, Toowoomba, Charleville, Port Headland, Katherine, Ballarat, Coober Pedy, Bourke, Albury… and your place!














